Blog
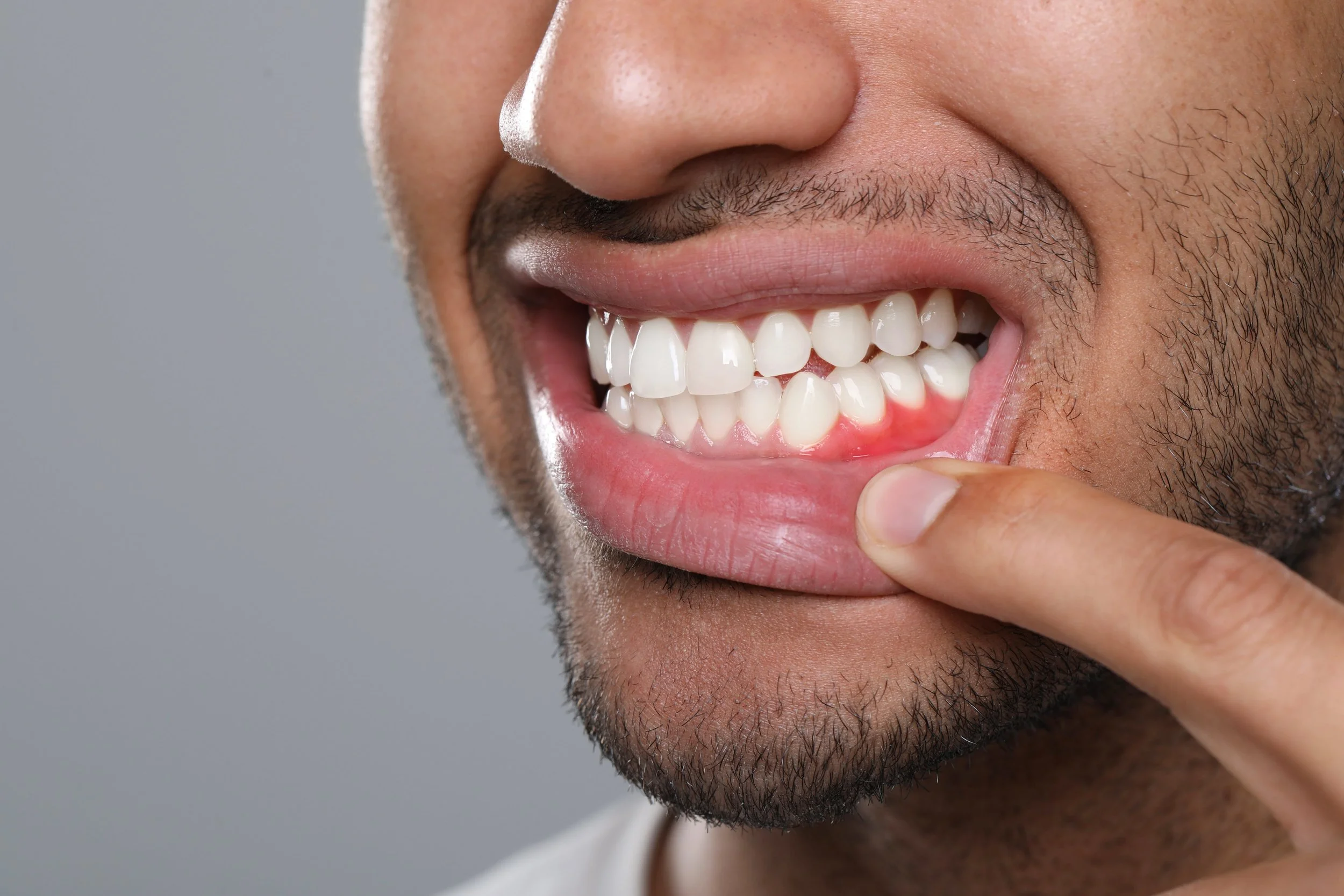
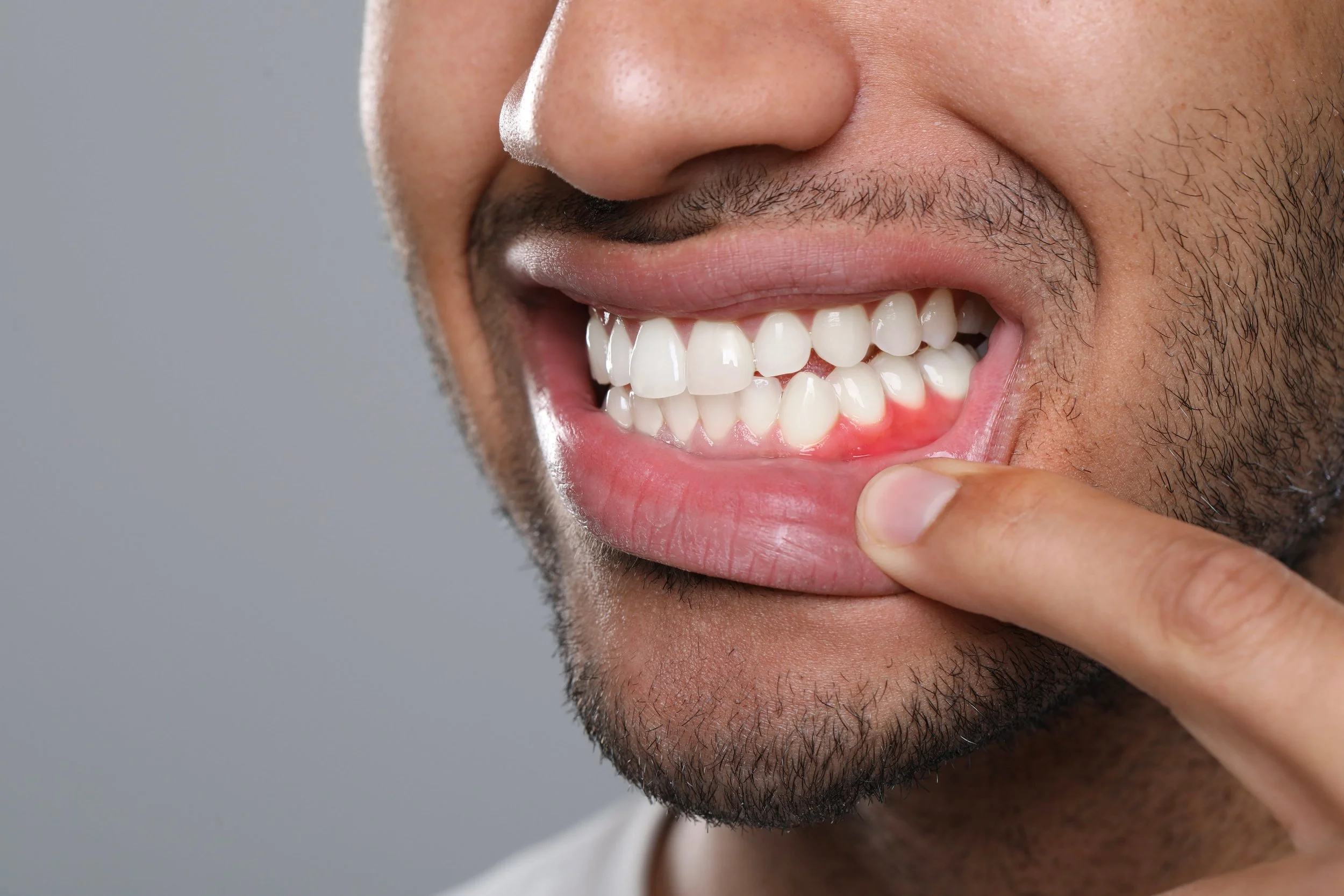
The Link Between Your Teeth and Your Overall Health
Discover how preventive dental care in Colorado protects more than your smile and why the connection between oral health and overall health matters.
Photo: andron19821982 via 123RF
Eating well. Getting enough sleep. Moving your body. Taking the right supplements. Those are usually the first things people think of when they’re trying to stay healthy.
Your dentist probably isn’t top of mind. But maybe they should be.
That’s because your mouth plays a much bigger role in your overall health than most people realize, and in some cases, it’s one of the first places your body signals that something isn’t quite right.
It works both ways, too. What’s happening in your mouth doesn’t stay there. Poor oral health can quietly influence the rest of your body over time.
There’s a growing body of research around the connection between oral health and overall health, linking conditions like gum disease to more serious systemic issues.
At Sanitas Family Dentistry, we look at preventive dental care in Colorado a little differently. Yes, clean teeth matter — but the bigger picture is your long-term health.
What Is the Mouth-Body Connection?
Your mouth isn’t just … your mouth. It’s an entire ecosystem. Inside it lives a complex community of bacteria known as the oral microbiome. Most of it is harmless. Some of it is even helpful. But when things get out of balance, that’s when problems arise.
If oral hygiene slips or dental issues go untreated, harmful bacteria can take over. The result is often inflammation, especially in the gums. Inflammation has a way of traveling — and it’s not a good thing!
Inflammation can affect the bloodstream and spread to other parts of the body, which is where the “mouth-body connection” really starts to matter.
That’s why oral health isn’t just cosmetic, it’s preventive — and more and more patients seeking dental care in Louisville, Boulder, Erie, Lafayette, and Superior are starting to think about it as a long-term health strategy, not just a short-term fix.
Gum Disease and Heart Disease: An Unexpected Link
This is the one that surprises people the most.
Gum disease and heart disease don’t seem like they should have anything to do with each other, but research suggests otherwise. Organizations, including the American Academy of Periodontology and the American Heart Association have highlighted the findings that there could be a big connection between periodontal disease and cardiovascular issues.
Here’s the simplified version of why: Gum disease is a chronic inflammatory condition. As it progresses, bacteria can enter the bloodstream and contribute to inflammation in other areas, such as the arteries.
Over time, that may play a role in the narrowing of the arteries, an increased risk of blood clots, and a higher likelihood of heart attack or stroke
It’s not as simple as cause and effect. But the relationship is strong enough that it shouldn’t be ignored. And it’s one more reason preventive dental care in Colorado matters.
The Two-Way Relationship Between Dental Health and Diabetes
If you’re managing diabetes, oral health becomes even more important. People with diabetes tend to be more prone to infections, including gum disease. At the same time, gum disease can make it harder to keep blood sugar levels stable.
So, it becomes a loop: Elevated blood sugar feeds inflammation, and inflammation makes blood sugar harder to control. Common signs to watch for include bleeding gums, bad breath that won’t go away, gum recession, or teeth that feel slightly loose.
This is where consistent, ongoing dental care really makes a difference, especially when it’s coordinated with your overall health management.
Pregnancy and Oral Health: Easy to Overlook, Important Not to
We don’t have to tell you that pregnancy changes your body a lot — your gums are often included in that list. Hormonal shifts can make them more sensitive, more reactive, and more prone to inflammation. Pregnancy gingivitis is common, but that doesn’t mean it should be ignored.
Photo: starik73 via 123RF
There’s also evidence linking untreated gum disease to complications like preterm birth and low birth weight.
The good news? Preventive dental visits during pregnancy are safe and strongly recommended. It’s one of those small things that can have a much bigger impact than people expect.
Your Mouth and Your Lungs
This one doesn’t get talked about enough.
Bacteria from the mouth can be inhaled into the lungs, which may contribute to respiratory infections like pneumonia, particularly in older adults or those with underlying conditions.
It’s another reminder that oral health is connected to systems most people wouldn’t immediately think of.
Inflammation Is the Throughline
If you zoom out, most of these connections come back to one thing: inflammation.
Inflammation is a natural response. But when it becomes chronic, it starts to create problems. Gum disease is one of the most common sources of chronic inflammation in the body, and because it’s often painless in the early stages, it can go unnoticed for a long time.
That’s where routine dental care really earns its keep.
When Your Mouth Is Trying to Tell You Something
Sometimes the signs are subtle, but sometimes they’re not.
If you’re noticing bleeding when you brush, persistent bad breath, sensitivity, or gum recession, it’s worth paying attention.
And it’s not just because of your teeth (which are important!), but also because of what it could be signaling more broadly.
Why Preventive Dental Care in Colorado Actually Matters
Most dental issues don’t show up overnight. They build slowly, quietly, over time. Preventive care is what interrupts that process.
Regular dental cleanings, exams, and screenings aren’t complicated — but they’re incredibly effective at catching problems early and keeping them from becoming something bigger.
And in many cases, they help reduce risks that go beyond your mouth.
How Often Should You Go to the Dentist?
Twice a year works for most people — but not everyone.
If you have a history of gum disease, diabetes, or other health considerations, you may need to come in more often. A good dental team will help you figure out what’s right for you, not just default to a standard schedule.
Choosing a Dentist Who Looks at the Bigger Picture
Dental care can be reactive or proactive. The difference comes down to approach.
The right provider isn’t just focused on fixing issues as they come up. That’s why the best dentists in Louisville, Boulder, Erie, Lafayette, and Superior are paying attention to patterns, prevention, and how your oral health connects to everything else.
That’s the philosophy behind Sanitas Family Dentistry. At Sanitas, preventive care isn’t an add-on — it’s the starting point. For every visit, our team focuses on early detection, personalized care, and long-term wellness. This is not just about quick fixes.
Patients seeking dental care in Boulder County may come in for a teeth cleaning but leave with a more complete picture of their health.
A Healthy Mouth, A Healthier You
It’s easy to think of dental care as separate from everything else, but it’s not. Your mouth is connected to your heart, your immune system, your metabolism — more than most people realize.
Taking care of it is one of the simplest ways to support your health over time. If it’s been a while since your last dental appointment, you’re not alone. It happens. But it’s also easy to start again.
Sanitas Family Dentistry offers preventive dental care across Louisville, Boulder, Erie, Lafayette, and Superior — so you can stay ahead of issues before they become something more.
Your Guide to Professional Teeth Whitening in Colorado
Is professional teeth whitening in Louisville, Boulder, Erie, Lafayette, and Superior worth it? Learn about costs, safety, results, and more in this guide.
Photo: milkos via 123RF
Many of us have looked in the mirror, caught our teeth in the wrong light, or seen a photo of our smile, and thought, “Hmm… maybe it’s time for a whitening refresh.” As professionals in the industry, we’ve been there, too.
Whether it’s coffee, tea, red wine, or just the normal wear and tear of life, no one is immune to teeth that lose a little sparkle over time. And while drugstore whitening strips and toothpaste promise the world, they do not always deliver the kind of bright, comprehensive results people really hope for.
The reality is that professional teeth whitening in Louisville, Boulder, Erie, Lafayette, or Superior can be a smart way to brighten your smile safely and effectively with guidance from a trusted dentist.
But is it actually worth it? And how does it compare to whitening at home? That is exactly what we are getting into here.
So What Is Professional Teeth Whitening, Really?
Professional teeth whitening is exactly what it sounds like — but with a big upgrade in safety, strength, and results.
At Sanitas Dentistry, we treat teeth whitening as a cosmetic dental treatment performed under a dentist's supervision, using professional-grade whitening agents that go way beyond what you’ll find at the store.
The goal is simple: Lift stains from deep within the enamel and brighten your natural tooth color in a noticeable, even way. And unlike DIY kits, everything is customized to your teeth, your sensitivity level, and your goals.
That personalization is where the real difference shows up.
Why Teeth Start Looking Less Bright Over Time
Nobody really warns you about this part of adulthood, but your teeth are quietly collecting stains, something they start telling you about via your smile. Here’s what usually causes that gradual dulling:
Coffee (yes, we’re looking at you)
Tea and soda
Blueberries (yes, this one surprises our patients!)
Red wine
Smoking or vaping
Certain medications
Natural aging and enamel thinning
Even with good brushing habits and rinsing after drinking coffee, tea, or wine, stains happen. Enamel also naturally becomes more translucent over time, allowing the yellowish dentin beneath to show through more easily. So if your smile has changed slowly over the years, you’re definitely not imagining it.
Dentist Whitening vs. At-Home Whitening
Many patients we see at our practice come to us for whitening advice because they have tried over-the-counter whitening strips, trays, or toothpaste and still didn’t get the results they wanted. Let’s break it down here, so you can understand what’s truly going on between at-home whitening and professional teeth whitening.
At-Home Whitening Kits
There are so many DIY options to choose from these days — from strips and gels to LED kits and whitening toothpaste. They’re popular because they’re easy, convenient, and inexpensive — but results vary a lot.
The biggest challenges we frequently see are uneven whitening (especially near gum lines), slower (and much more subtle) results, a higher chance of sensitivity, and a one-size-fits-all approach that doesn’t actually fit all.
These treatments may help a little, but it's rare for them to deliver a dramatic change that many people desire.
Custom Bleach Trays from a Dentist
With custom bleach trays, your dentist creates trays that are molded to your teeth and paired with professional-strength whitening gel. In our experience, people like this option because they deliver predictable results with more even coverage across all teeth. They’re also safer for gums and enamel.
It’s a nice middle ground between the convenience of over-the-counter treatments and solid results.
In-Office Professional Whitening
This is the “let’s do this in one visit” option. In-office professional teeth whitening in Colorado is the fastest way to see a noticeable difference, often several shades brighter in about an hour.
Our patients gravitate to this option when they want immediate results from stronger whitening agents. And, of course, it’s all supervised by a dental professional with customized protection for sensitivity.
If you want a visible transformation quickly — think events, photos, weddings, or just a reset — this is usually the most effective route.
What Actually Happens During a Whitening Appointment?
Photo: peopleimages12 via 123RF
If you’ve never had professional teeth whitening before, it’s normal to feel a little unsure and anxious about the process. But it’s actually very straightforward and painless. Here’s a quick overview of some common things to expect, whether you come to our dentistry practice in Colorado or another local dentist.
Have a short consultation: Your dentist will check your teeth and any existing dental work, as well as your overall oral health, to ensure you’re a good candidate for teeth whitening.
Pick your whitening method: You’ll choose between professional in-office whitening, take-home custom whitening trays, or a combination of both.
Begin the whitening procedure: For in-office sessions, your teeth are prepared and cleaned for the procedure, and your gums are carefully protected. Then, the whitening gel is applied and activated. The next thing you know (usually within one hour), your smile has brightened in real time.
At Sanitas Dentistry, we use the innovative Biolase Laser White system, widely considered the gold standard for teeth whitening. It is designed to be faster and cause less sensitivity than traditional methods, and we generally see it achieve 6-12 shades of whitening in under an hour.
Follow the aftercare tips: You might be told to avoid coffee, red wine, and dark foods for a few days to help your results fully settle in.
How Much Does Professional Teeth Whitening Cost in Colorado?
Let’s talk numbers, because this is usually part of the decision. In general, teeth whitening in Colorado falls into these ranges:
Drugstore kits: $20–$100
Custom bleach trays: $200–$400
In-office professional whitening: $400–$800
At first glance, professional whitening appears much more expensive. But if you add up how much you’ve spent on unsuccessful whitening strips, kits, and toothpaste options, you might be surprised by your investment!
Many of our patients have found professional teeth whitening to be more cost-effective over time because the results last longer — and it actually works. The outcome is more predictable. Think about it as less “try five products and hope for the best” and more “get it done right once.”
How Long Do Results Last?
With good habits, professional whitening results can last from 6 months to 2 years. To help your results last longer, you can avoid those teeth-staining beverages (sorry, coffee!) or make sure to rinse your mouth or brush your teeth immediately after consuming them. Drinking out of a straw can help, too.
You’ll also want to keep up with regular cleanings and brush and floss consistently. This is where some of those whitening toothpaste products and strips can help maintain the professional whitening results you’ve achieved.
Who Is a Good Candidate for Whitening?
You’re likely a good fit if you have healthy teeth and gums, want a noticeably brighter smile, are unhappy with surface-level staining from food or drinks, or are preparing for a big life moment or photos.
You may need a different approach if you have untreated cavities or gum disease, have crowns or veneers on your front teeth (these don’t whiten), or experience significant tooth sensitivity.
A consultation with a dentist in Louisville, Boulder, Erie, Lafayette, or Superior can help clarify what’s realistic for you.
Is Teeth Whitening Safe?
The short answer? Yes — when done correctly. A lot of people worry about the safety of teeth whitening, and it’s a fair question. Whitening is safe when it’s supervised by a qualified dental professional and tailored to your oral health.
Working with a trusted dentist in Boulder, Louisville, Erie, Lafayette, or Superior helps ensure that your gums stay protected, your tooth enamel isn’t overexposed, any sensitivity is properly managed, and that the whitening level is appropriate for your teeth.
Most issues people worry about — like burning, uneven whitening, or severe sensitivity — typically stem from overuse of store-bought products or poorly fitting trays. These issues often don’t arise from professional care.
So… Is Professional Teeth Whitening Really Worth It?
For most people, the answer here is “yes.” We’ve never had a patient at our practice regret making this small investment in their smile.
Here’s the simplest way to think about it: If at-home whitening is like slowly painting a room with a small brush, professional whitening is like hiring someone who knows exactly how to get it done evenly, quickly, and beautifully.
You’re investing in better results, safer application, less trial and error, and a noticeably brighter smile. And for many patients, that confidence boost is the real payoff.
If you’ve been considering professional teeth whitening from a dentist in Louisville, Boulder, Erie, Lafayette, or Superior, we can help.
At Sanitas Dentistry, whitening is never one-size-fits-all; it’s highly personalized. We offer the most top-of-the-line innovative, safe, and highly effective solutions, including custom bleach trays with Opalescence, Opalescence Go Trays, and in-office whitening featuring the Biolase Laser White system.
These solutions are thoughtfully tailored around your goals. Whether you want a subtle refresh or a big confidence boost, the right plan makes all the difference. We love helping our patients get their smiles back to their brightest selves.
Why Are My Gums Bleeding? Causes, Prevention, and Treatment
Wondering “why are my gums bleeding when I brush?” Learn the common causes behind bleeding gums and treatment options to protect your oral health.
Photo: liudmilachernetska via 123RF
Brushing your teeth shouldn’t make your sink look like a crime scene. And flossing shouldn’t trigger a bloody mouth. But if you’ve ever noticed some pink in the sink while brushing, you’re not alone, and you’re probably wondering: Why are my gums bleeding?
Many people ignore the bleeding or assume it’s just a normal thing that happens. Others start to worry that it could be a sign of something serious. The truth? Well, it lies somewhere in between.
Bleeding gums are relatively common, especially when flossing, and we get asked about this condition a lot at Sanitas Family Dentistry. But just because it’s common doesn’t mean it’s normal. Bleeding gums are your body’s way of signaling that something in your oral health needs some attention.
In many cases, bleeding gums can easily be remedied with simple changes to your oral hygiene routine, along with professional care. But sometimes, they may point to something more serious, like early gum disease or other underlying issues.
In this guide, we’ll explore why gums bleed, what causes gum inflammation, when to see a dentist, and what you can do to protect your gum health.
Why Are My Gums Bleeding When I Brush?
If you’re asking yourself, “Why are my gums bleeding?” (or consulting Dr. Google or Dr. ChatGPT for the answers), here’s what you need to know. Several factors could be causing this issue for you. Some are related to oral hygiene habits, while others could stem from health conditions or lifestyle factors.
Plaque Buildup and Gingivitis
One of the most common causes of gum bleeding is plaque buildup along the gumline, which can lead to gingivitis. Plaque is a sticky film of bacteria that may not always be removed thoroughly enough during brushing and flossing, and it can irritate the gums.
Over time, that irritation turns into actual inflammation, which can make the gums red, swollen, and more likely to bleed during brushing or flossing. This is actually an early stage of gum disease called gingivitis, which many patients at our practice are surprised to learn.
The good news is that this initial stage of gum disease is reversible when caught early, which is why we encourage our patients to pay attention to small signs like bleeding, as well as other gingivitis symptoms such as red or swollen gums, tender gums, persistent bad breath, and gum sensitivity.
If left untreated, gingivitis can progress into periodontal disease, a far more serious condition that can damage the bone supporting your teeth. It’s also a main cause of tooth loss in adults.
Brushing Too Hard or With the Wrong Toothbrush
Another common cause of bleeding gums when brushing is being a little too aggressive in your brushing technique. Try to remember not to take out your stress on your teeth! Brushing with gentle and thorough circular motions across all your teeth — the front and the back — is important to remember.
If you’ve recently purchased a new toothbrush and noticed some extra sensitivity or bleeding, your brush may be too firm, and your gums are noticing. Both hard bristles and applying too much pressure with a softer bristle can irritate gum tissue and cause minor bleeding.
At Sanitas, we almost always recommend softer bristles or an electric toothbrush to moderate the intensity of your brushing. Regardless, both options will be much gentler on the gums.
Beginning a New Flossing Routine
Flossing is incredibly important to your oral health routine, but if you’ve just recently started flossing regularly, you may notice some bleeding at first as your gums adjust.
This often happens because the gums are slightly inflamed due to plaque buildup between the teeth. As flossing removes the plaque and bacteria, the gums begin to heal, and the bleeding should dissipate.
Photo: brizmaker via 123RF
In most cases, the bleeding improves or stops within about a week of consistent flossing. If it continues longer, it’s worth consulting a dental professional.
However, improper flossing technique can also cause some bleeding. Try not to “snap” the floss in between your teeth. Use a gentler in-and-out motion, or consider a water flosser, which is also helpful if you have any orthodontics that make it difficult to manage traditional string floss.
Medical Conditions or Medications
Some health conditions, like diabetes and immune health disorders, and pharmaceutical drugs, including blood-thinning medications, hormonal birth control, and even aspirin and NSAIDs, can make your gums more prone to bleeding.
In our practice, we always ask patients about their current medications, which is why it’s important to always keep your dentist informed about any changes in prescriptions or over-the-counter medications you take regularly.
Hormonal Changes
For female patients experiencing gum bleeding, it’s possible that some hormonal shifts could be making their gums more sensitive and prone to bleeding. That’s because hormones increase blood flow to gum tissue, which can make gums react more strongly to plaque buildup.
This is most common during times like puberty, pregnancy, and menopause, when hormonal fluctuations are more extreme.
Vitamin Deficiencies
Certain vitamins and nutrient deficiencies can also contribute to gum inflammation and bleeding. The most common include Vitamin C deficiency and Vitamin K deficiency. Vitamin C helps strengthen your immune system, right along with your teeth and bones, while Vitamin K helps your blood clot properly.
A balanced diet rich in fruits, vegetables, and whole foods can help support healthy gums.
Smoking and Vaping
Smoking and vaping have a host of negative health consequences, and your teeth and gums are not immune to the effects either. Both practices can increase your risk of oral health problems, not the least of which are sensitive and bleeding gums.
Your sensitive gums could also be a simple vitamin deficiency, especially Vitamin C and Vitamin K.
For example, Vitamin C can boost the immune system while strengthening your bones and teeth. A lack of Vitamin K can prevent your blood from clotting properly, making your gums more susceptible to bleeding.
How to Stop Bleeding Gums
If you’re wondering how to stop bleeding gums, the good news is that many cases can be improved with better oral care and healthy habits. Here are some of the most effective strategies we like to remind our patients about:
Focus on Brushing Well: We all know it’s important to brush twice a day, but make sure you use a soft toothbrush and don’t forget to gently focus on the gumline, where plaque tends to accumulate.
Floss Daily: You only have to floss once per day, but that’s more than many people want to do. But daily flossing is so important for removing plaque between your teeth that brushing just cannot reach.
Eat a Well-Balanced Diet: We’ve all heard to avoid sugar for teeth, but it goes beyond that for your best oral and gum health. Nutrients play a big role, so make sure to eat the rainbow and introduce foods rich in vitamin C, calcium, and antioxidants to support strong gum tissue and reduce inflammation. Your whole body will thank you!
Schedule Bi-Yearly Appointments: Even the best oral care needs a little TLC from the dentist. Professional cleanings every six months are highly advisable to remove plaque buildup that brushing cannot reach, keep gums healthy, and catch minor issues before they become major problems.
How We Diagnose Gum Problems
At Sanitas, we begin with a comprehensive evaluation that explores all health factors related to a patient's oral health and bleeding gums.
Patients can expect the exams to include checking for signs of inflammation, evaluating plaque and tartar buildup, measuring the space between teeth and gums, and taking X-rays, if needed. We’ll also perform a thorough teeth cleaning.
Taken together, this allows our team to determine whether the bleeding is caused by gingivitis, early periodontal disease, or another oral health issue entirely.
How We Help Patients with Their Oral Health
Many cases of bleeding gums are relatively minor and can be remedied with a few easy fixes to your daily routine. But if your gums continue to bother you and you still find yourself asking, “Why are my gums bleeding?”, it’s time to make an appointment with your dentist to investigate the problem.
If you’re looking for a Colorado dentist in Louisville, Boulder, Erie, Lafayette, or Superior, Sanitas Family Dentistry can help. At our practice, we provide comprehensive dental exams, professional cleanings and gum disease treatment, advanced diagnostic technology, personalized oral health guidance, and more.
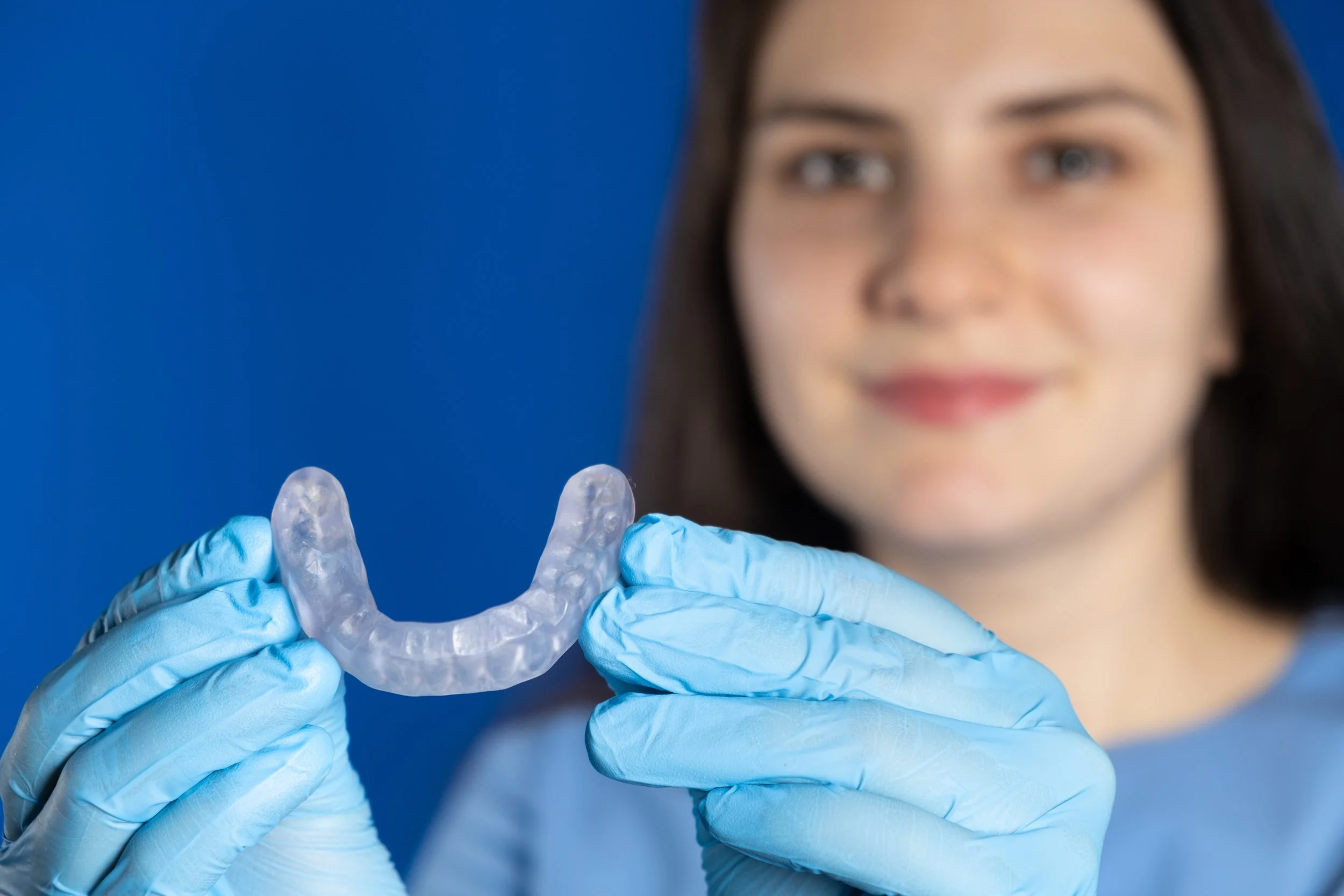
What's the Difference Between Night Guards and Mouth Guards?
How does a night guard work? Learn how dental night guards protect teeth and how they’re different from mouth guards, plus costs, cleaning tips, and more.
Photo: serezniy via 123RF
Night guards and mouth guards are both protective measures for your teeth — kind of like a helmet is for your head. But that’s where the similarities stop.
While night guards and mouth guards are often grouped together because they look similar to each other, they serve very different purposes. One is designed to protect your teeth from nighttime grinding and clenching. The other is meant to prevent injury during sports.
At Sanitas Dentistry, we regularly help patients across Louisville, Boulder, Erie, Lafayette, and Superior understand the differences between a night guard and a mouth guard, and whether either one is right for them.
In this guide, we’ll walk through what night guards do, how they’re different from mouth guards, and how they may be able to help you.
What Is a Night Guard?
A night guard for grinding teeth is a dental appliance that’s worn only while you sleep. Sometimes referred to as an occlusal splint, occlusal guard, or bite splint, it creates a protective barrier between your upper and lower teeth to prevent any damage caused by clenching and grinding — a condition known as bruxism.
Because bruxism often happens unconsciously during sleep, many of our patients at Sanitas Dentistry don’t even realize they grind their teeth. Others may wake up in the morning with a headache or experience soreness and stiffness in their jaw, without initially understanding why.
Dentists can detect even subtle signs of bruxism, like worn enamel or small fractures, gum recession caused by pressure, or jaw inflammation. All these clues could point to teeth grinding.
How Does a Night Guard Work for Grinding Teeth?
While many people may grind their teeth from time to time, especially during highly stressful times, it becomes a concern if signs and symptoms point to repeated grinding.
That’s where a dental night guard comes in.
A dental night guard works in several ways, and most patients notice the difference pretty quickly.
It acts as a shock absorber of sorts.
Think of the guard like a cushion or a barrier between your upper and lower teeth. Instead of enamel grinding directly against enamel, the guard absorbs all that pressure. Over time, this is what helps prevent cracks, chips, and the gradual flattening of your teeth.
It distributes pressure evenly.
People don’t often grind their teeth uniformly — certain teeth take the brunt of it. So, a night guard spreads that pressure out more evenly, again protecting your teeth.
It relaxes the jaw muscles.
Many patients are also really happy to find that their jaw feels more relaxed during the day once they start wearing a night guard. The guard slightly changes how your teeth come together, which can decrease the intensity of your grinding and clenching. Less intensity often means fewer morning headaches and reduced jaw stiffness and facial soreness.
It protects dental work.
If you have crowns, veneers, implants, or orthodontics, a night guard adds an extra layer of protection for that dental work in addition to your natural teeth.
It’s important to know that the night guard won’t actually stop teeth grinding, but it does mitigate any short-term and long-term effects of bruxism by protecting your teeth and jaw.
Photo: garnazarina via 123RF
An Important Distinction Between a Mouth Guard and a Night Guard
A mouth guard, sometimes called a sports guard, is also protective, but it’s designed to protect your teeth from a completely different type of force.
While night guards mitigate the negative effects of prolonged grinding, mouth guards are designed to absorb sudden impacts, such as a hit during football, boxing, or martial arts.
Mouth guards are typically thicker and bulkier because they need to cushion teeth against trauma. While they’re excellent for preventing chipped or knocked-out teeth during athletic activity, they’re not designed to address nighttime grinding or jaw tension.
This is where confusion can arise. Patients sometimes purchase a sports mouth guard hoping it will solve their grinding problem. Unfortunately, it usually doesn’t provide the right type of protection and can even feel uncomfortable during sleep because it’s so much bigger than a night guard.
How Much Is a Night Guard from the Dentist?
One of the most common questions — and even concerns — we hear is: How much is a night guard from the dentist?
While you can purchase a relatively inexpensive night guard off the shelf at a drugstore, we really encourage our patients to invest in a professional, custom-fitted night guard. We see the best results with guards that are personally designed to fit your mouth.
While pricing varies based on materials and customization, these options will cost more than over-the-counter options because they use impressions or digital scans for personalization. But that extra investment means the night guard will be more durable, more comfortable, and longer-lasting; plus, it’s generally more effective because it’s designed for your specific mouth and bite alignment.
In our experience at Sanitas Dentistry, many dental insurance plans provide partial coverage for a night guard when it is deemed medically necessary. We walk patients through options and provide fair and transparent pricing so there are no surprises down the line.
Are Night Guards Worth It?
From a clinical standpoint, the answer is absolutely “yes,” especially if grinding is already causing damage to your teeth.
Many patients hesitate because they’re unsure about the cost or wonder if they should just buy something over the counter. But when you compare the price of a custom dental night guard to the cost of repairing damaged teeth or replacing crowns, the value becomes clear.
When we talk with patients who are evaluating whether a night guard is worth it, we’ve often found it helpful to help them reframe the question. Instead of, “Is this necessary?” make sure you’re also answering the question: “What happens if I do nothing?”
In many cases, the ongoing daily discomfort and the long-term cost of untreated grinding are significantly higher.
How Often Do You Have to Replace Night Guards?
With the right TLC, a night guard can last you for at least a few years before you may need to replace it. The actual timeline depends on the severity of your bruxism and how well the guard is maintained.
If you grind heavily, you may wear out the appliance more quickly. But this is actually a good thing — because it means the guard is absorbing the force instead of your teeth!
Regular checkups will allow your dentist to monitor wear and recommend a replacement when necessary.
How to Clean Night Guards Naturally
Speaking of TLC, proper care extends the life of any appliance, including night guards, while protecting your oral health. If you’re wondering how to clean night guards naturally, the process is quite easy.
Every morning, rinse the guard with water and gently brush it with a soft toothbrush. Then, put it in a safe place to dry.
For deeper cleaning, about once a week, soak the guard in a diluted vinegar solution or hydrogen peroxide to help remove any buildup. Avoid hot water, as it can warp the material. And whatever you do, do not place it in the dishwasher!
Where to Get a Night Guard
Now that you can answer the question, “How does a night guard work?,” you may be ready to take the next step.
If you’re looking for where to get a night guard in Louisville, Boulder, Erie, Lafayette, or Superior, Sanitas Dentistry is here to help.
We begin the process with a comprehensive consultation and evaluation to listen to your symptoms, assess for signs of tooth wear, evaluate your bite, and determine whether grinding is contributing to any discomfort or enamel damage.
If we decide that a night guard is right for you and you want to move forward, we take impressions to create a precise fit. Once your guard is ready, we ensure it fits comfortably and make any adjustments.
Because bruxism is often a long-term habit, ongoing attention and care matter — and it’s something we keep an eye on during every routine six-month cleaning and exam.
Remember: A well-fitted guard today can eliminate the side effects of bruxism and prevent significant restorative treatment in the future.
Are Dental Implants Worth It? A Guide for Colorado Patients
If you’ve wondered “are dental implants worth it,” this guide will help you determine whether they make sense for your health, lifestyle, and long-term goals.
Photo: seventyfour74 via 123RF
Losing a tooth when you’re a child is all fun and games, especially when the Tooth Fairy paid a visit. But missing a tooth as an adult? That’s a whole different story.
Missing a tooth (or several teeth) as an adult is a common dental problem, though. And it’s one that obviously affects your smile and how confident you feel about your smile in everyday moments. But it can affect far more than that, too. It can change how you eat and drink, how you speak, and even your overall oral health.
If you’re exploring tooth replacement options, you’ve probably found yourself asking a very practical (and very valid) question: Are dental implants worth it?
For many patients, dental implants are considered one of the most effective and long-lasting solutions available. But they do require a greater investment of time and money than alternatives like bridges or dentures.
This guide is designed to help you understand what dental implants really are, how they compare to other options, and whether they make sense for your health, lifestyle, and long-term goals.
What Are Dental Implants? (in Plain English!)
When patients hear the phrase dental implant, they often imagine something bulky or mechanical. But actually, implants are surprisingly simple in concept, and very practical in everyday life.
Instead of just replacing the part of the tooth you see, a dental implant replaces the root as well. That’s what makes it different from bridges or dentures, and it’s also why many patients say it feels more “real” once everything is healed.
A dental implant starts with a small titanium post that’s placed into the jawbone. Titanium is used because the body accepts it well — something we often explain to patients who are understandably nervous about a foreign material in their mouth.
Over time, the bone grows around the implant and holds it in place. When patients hear this, they usually pause and say something like, “Wait. It actually becomes part of my bone?” And yes, essentially, it does — as weird as that might sound!
Once that healing phase is complete, the visible tooth, which is called the crown, is added on top. At that point, most patients stop thinking of it as an implant and start thinking of it as just… their tooth.
The Elements of a Dental Implant (and Why They Matter)
At Sanitas Family Dentistry, we find it helps patients understand implants a bit better by breaking them down — not because the process is complicated, but because knowing what’s happening reduces that sense of uncertainty and anxiety.
A dental implant has three main parts:
The implant post, which is the titanium “root” placed in the jawbone
The abutment, which connects the implant to the replacement tooth
The crown, which is the part you see when you smile
Patients are often most focused on the crown: how it will look, whether it will match, and whether people will notice it. In practice, that’s usually the easiest part. Today’s crowns are custom-made to blend in naturally, and once they’re in place, even patients tend to forget which tooth was replaced.
The real work happens beneath the surface, where the implant post bonds to the bone through a process called osseointegration. We won’t get overly scientific here, but this step is what gives implants their long-term strength and stability.
What the Dental Implant Process Is Actually Like
One of the biggest misconceptions we hear is that getting a dental implant is a single, intense procedure. Instead, it’s a series of steps intentionally spaced out over time.
Here’s how it typically unfolds:
1. Consultation: This is where we listen to your concerns and assess your oral health. Imaging and exams help determine whether implants are a good option, but the conversation matters just as much to address questions and concerns. Dental implants are generally suitable for most patients who have lost one or more teeth and have sufficient bone density to support the implant
2. Implant Placement: The implant itself is placed during a minimally invasive surgical procedure. We work with exceptional implant placement experts. And while many patients dread this step the most, they are often surprised by how manageable it is. A common comment we hear afterward is,“That was it?”
While there will be some mild swelling and soreness for a few days post-procedure, most patients experience hardly any disruption to their daily activities.
3. Post-Placement Healing: This is the part that patients actually find the hardest! And that’s because it requires a little bit of patience. Over the next few months, there is a waiting game before the permanent implant can be placed. During this time, the implant bonds with the jawbone. It’s not the most exciting phase, but it’s critical for long-term success.
4. Crown Placement: Once the implant is fully bonded and integrated to the jawbone, the custom restoration — a.k.a. the crown — can be placed. This is when patients feel like their smile is finally “complete” again.
Dental Implants Compared to Other Tooth Replacement Options
Dental implants, bridges, and dentures can all replace missing teeth, but they do it in very different ways — and those differences tend to matter more over time than patients initially expect.
Photo: zinkevych via 123RF
Considerations for Dental Bridges
A dental bridge essentially replaces a missing tooth by attaching an artificial tooth to the teeth on either side of the gap. Bridges generally cost less upfront and can be completed more quickly than dental implants. That’s often a good thing for patients who want a quick fix or to avoid surgery.
But the downside is that bridges can potentially have a negative impact on healthy teeth. To place a bridge, the neighboring teeth typically need to be reshaped to support it.
Here’s a quick summary about dental bridges:
Lower initial cost
Faster overall treatment timeline
Often requires reshaping healthy adjacent teeth
Typically lasts 7 to 10 years before replacement
Considerations for Dentures
Dentures get a bad rap — but there’s a reason they’ve been commonly used for decades. They do work. Dentures can be partial or full, and they’re a reasonable option for some. Both partial or full dentures are generally more affordable and can be removed for cleaning. But dentures can also come with challenges that aren’t always anticipated.
For example, we often hear concerns about slipping, clicking, or needing adhesive to feel secure. Some patients also notice changes in their speech or the pronunciation of certain words. Others tend to avoid certain foods because chewing doesn’t feel as stable as it did before.
Here’s a quick summary about dentures:
Lower initial cost
Ease in cleaning, because they’re removable
May slip or feel unstable in the mouth
Could affect speech and eating
May accelerate bone loss in the jaw over time
May require replacements or repairs and adjustments over time, increasing the cost
Considerations for Dental Implants
While they’re more expensive, dental implants deliver a more permanent solution than both bridges and dentures. Because they’re secured in the jawbone, they don’t move or shift. Patients don’t need adhesives, and most say they stop thinking about their teeth altogether once the healing process is complete.
Here’s a quick summary about dental implants:
Higher initial investment
No adhesives required
Don’t alter neighboring teeth
Support jawbone health and preserve facial structure
Natural look and feel that provides improved comfort and confidence
Can last 20 years or more
Many patients who work with a dentist in Colorado for dental implants choose them because they offer many advantages in both the short and long term.
The Cost of Dental Implants in Colorado
Because the main drawback of dental implants is their cost, it’s not surprising that cost is one of the most common — and understandable — questions patients ask.
The cost of dental implants in Colorado can vary based on several factors, including how many teeth are being replaced, whether bone grafting or other preparatory procedures are needed, and the type of final restoration being placed. A single implant is very different from a full-arch solution, and materials and technology can also influence pricing.
At Sanitas Family Dentistry, we offer clear, transparent, and fair pricing to go along with a personalized treatment plan. The goal is to eliminate any surprises and help patients make informed decisions that feel right for them.
So… Are Dental Implants Worth It?
For many people, dental implants are worth it — but not because they’re the newest or most advanced option. They’re worth it because they solve multiple problems simultaneously.
Implants restore chewing strength so you can eat what you want, when you want, protect the jawbone, and eliminate the daily inconveniences of removable options. We often hear from patients who wish they had done implants years ago, especially after struggling with dentures or replacing a bridge multiple times.
That said, the concept of “worth” is highly personal. What makes sense for one patient may not make sense for another, and that’s okay.
Why Patients Choose Sanitas for Dental Implants
Whether you’re searching for dental implants in Colorado, researching options in Superior, Boulder, Louisville, or Erie, or simply Googling dental implants near me, this guide has helped you feel more informed (and more confident!) about your next steps.
And if you are looking for an option for dental implants near Superior, Boulder, Louisville, Lafayette, or Erie, Colorado, Sanitas Family Dentistry delivers the highest level of experience and care.
Our team always prioritizes a patient-first approach that focuses on both comfort and education. From the initial consultation to the final placement of the restoration, our team and dental implant specialist in Colorado guide patients every step of the way.
At Sanitas Family Dentistry, we are not only known for our modern techniques and state-of-the-art materials, but also for personalized evaluations and customized treatment plans. We provide clear, honest communication at every stage in a calm, supportive environment.